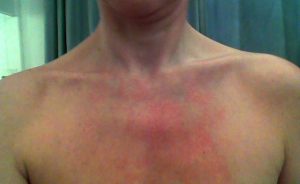
Mast Cell Activation Disorder—Symptoms and Causes
Abdominal pain, intestinal cramping, burning pain, cough, conjunctivitis, difficulty focusing, headache, hives—and the list goes on. For patients with MCAD, life is a continuous pinball machine of symptoms blasting from one organ system to the next.
Mast Cell Activation Disorder (MCAD) is a complex condition that can cause disruption everywhere from the gastrointestinal tract and skin to the cardiovascular respiratory and neurological system.
What is a “Mast Cell?”
Mast cells can be found all over the body and play a key role in your immune system. These cells are filled with granules that can release histamine, heparin and prostaglandins when they’re signaled appropriately. IgE can trigger this release in allergic reactions and anaphylaxis shock. You can find mast cells most commonly in the tissue that surrounds blood vessels and nerves—usually near the skin, GI tract, in the mucosa of the lungs, as well as in the nose, conjunctiva and mouth.
Systemic Mastocytosis is a disorder that is caused be a genetic mutation that results in a vast number of mast cells populating the body. While these cells are supposed to help protect the body from disease and aid in healing—an excess of mast cells can build up in sensitive tissues, overwhelming your body and causing everything from facial flushing to loss of consciousness.
There are several different kinds of Mast Cell Disorders The World Health Organization (WHO) classification (simplified here) is:
- Cutaneous mastocytosis – usually children.
- Urticaria pigmentosa (maculopapular cutaneous mastocytosis) – the most common type.
- Diffuse cutaneous mastocytosis (very rare).
- Mastocytoma of skin.
- Systemic mastocytosis:
- Indolent systemic mastocytosis
- Systemic mastocytosis with associated haematological non-mast cell lineage disease (SM-AHNMD).
- Aggressive systemic mastocytosis.
- Mast cell leukaemia (very rare).
- Localised mast cell proliferations (very rare).
- Extracutaneous mastocytoma.
- Extracutaneous mast cell sarcoma.
Telangiectasia macularis eruptiva perstans (TMEP) is a rare form of cutaneous mastocytosis, in which telangiectasia occur together with the rash.[4]
(http://www.patient.co.uk/doctor/Mastocytosis-and-Mast-Cell-Disorders.htm)
Symptoms of Mast Cell Activation Disorder can include:
- Malabsorption
- Eye Discomfort
- Headache
- Decreased or increased bone density
- Muscle pain
- Bone Pain
- Episodes of low blood pressure and syncope
- Anaphylaxis
- Ear, nose and throat inflammation
- Infections such as bronchitis, rhinitis and conjunctivitis
- Food/Drug Intolerances
- Diarrhea
- Nausea and Vomiting
- Abdominal Pain
- Skin Lesions
- Itching
- Fatigue
(http://www.patient.co.uk/doctor/Mastocytosis-and-Mast-Cell-Disorders.htm)
Mast Cell Diagnosis
How is MCAD diagnosed? Most often—it isn’t. The truth being that because the disease mimics so many others—and is so difficult to test for, a clinical diagnosis is generally what is found. However, there are certain methods of diagnosing available.
Biopsy
Patients who have the clinical diagnosis of Mast Cell can get a diagnosis through a biopsy of the lining of the intestinal track. Mast Cells normally reside in this tissue, because most allergins come in through the intestinal track.
Serum-Histamine Level
Histamine is a substance that is released from specialized cells called mast cells when they are activated, often as part of an allergic immune response. This test measures the amount of histamine in the blood or urine. The most accurate results come from when the serum histamine level is drawn during the attack.
Chromogranin A Test
Other tests that may be done which are somewhat specific for Mast Cell Activation Syndrome include serum chromogranin A (in the absence of cardiac and renal failure, neuroendocrine cancer, and proton pump inhibitor use) and serum and urinary leukotriene and prostaglandin isoforms.
How is MCAD Treated?
MCAD’s treatment focuses on managing it’s symptoms. Here are a few options to treat the symptoms of MCAD:
- Antihistamines| | Antihistamines can greatly improve quality of life for those with MCAD
- Singulair | Singulair is a prescription medication that helps prevent and control asthma attacks, including attacks caused by exercise. Also treats seasonal (short-term) and perennial (long-term) allergies.
- Trigger Avoidance | If patients can identify which food, environmental causes, or medications are causing their allergy—they can avoid these triggers to help prevent attacks in the future.
- Avoiding Overheating | Patients with MCAD should avoid overheating, which can cause or exacerbate attacks.
- Gastrocrom (Cromolyn) | A prescription medication called “Gastrocrom” (Cromolyn) s used in people with a food allergy to prevent serious reactions to foods. It is also used to treat and prevent inflammatory bowel diseases (e.g., ulcerative colitis). Cromolyn belongs to a class of medications called mast cell stabilizers. It works by preventing mast cells (cells involved with allergic/inflammatory reactions) from releasing substances (e.g., histamines) that can cause skin and gut problems.
Please note that this is an introductory article to Mast Cell and we encourage patients to continue their research when it comes to this complex and difficult to diagnose condition. For more information on Mast Cell conditions continue reading here: